Interactive Early Learning Solutions Backed by Research
Since 1984, Hatch has partnered with educators to extend their impact and address learning loss through purposeful practice and data stories.
Extend teachers' reach with engaging digital learning tools
When unified, the Hatch suite creates a complete classroom solution for accelerating student learning across seven domains of learning with a focus in math, literacy, and social-emotional development.
Transform Early Learning with Hatch’s Interactive Suite of Solutions


Ignite by Hatch™
Ignite by Hatch™ is our dynamic digital learning platform that captivates and engages early learners while seamlessly providing critical academic and child development data to teachers and administrators. Aligned with standards and backed by research, Ignite promotes growth in multiple domains of learning.

IgniteTable by Hatch™
IgniteTable by Hatch provides a collaborative learning experience for children to engage with peers while building social-emotional learning, communication, and prosocial skills. As young learners play, IgniteTable automatically captures authentic work samples and data so teachers can spend less time administering SEL assessments and more time focusing on the specific SEL skill areas that are crucial for each child’s success in school and beyond.
IgnitePanel by Hatch™
IgnitePanel by Hatch™ is a game-changing interactive panel software solution that revolutionizes early childhood classroom instruction thanks to its inclusion of standards-aligned early learning lessons and activities. Educators can effortlessly plan and implement research-based activities tailored to individual learners. Hatch’s software is loaded with hands-on, engaging, and developmentally appropriate content that enables teachers to foster truly collaborative learning experiences. IgnitePanel is the ultimate whole-class solution.

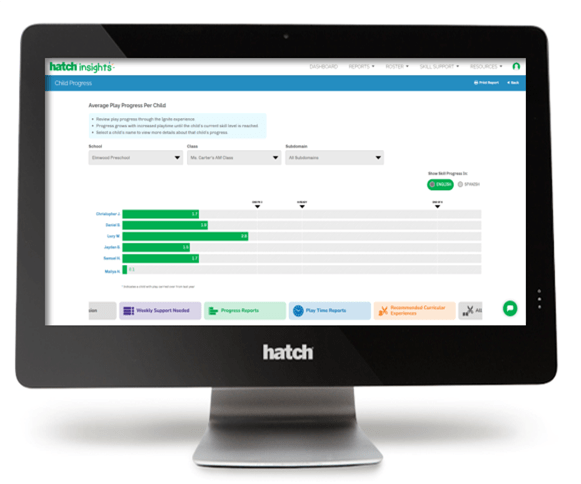
Insights by Hatch™
Through the robust Insights by Hatch™ administrator and teacher dashboards, powerful data stories are readily available to inform classroom instruction and assess student growth. Real-time data and reports from both Ignite by Hatch™ and IgniteTable™ extend teachers' ability to collect objective evidence for assessment and support children through personalized instruction. Hatch Insights also includes many supplemental resources for learning outside of the classroom, as well as snapshots of both school-wide and class activity.




